This is an acute laminitis case that was initially painful and exhibiting the typical founder stance on December 16 2012. No known cause but a mild colic episode had occurred 3 days prior. I was able to perform venograms on what I would consider Day one of laminitis. These plain film radiographs and venograms create a baseline in which to compare follow up venograms. This allows assesment of the mechanical therapy applied and severity of compromise in the days to follow. Venograms 5 days later show moderate compromise already. Consider the amount of compromise present while treated with mechanics. Unloading the Deep flexor tendon, its forces applied to the dorsal lamellar zone and sole directly below tip of coffin bone via raising the palmar angle.
There is no measurable displacement of the bone but significant change has occured within the vascular network as early as five days. Some financial constraints existed and it was decided to wait 30 days and repeat venograms to evaluate if the mechanics applied would be enough. I warned the client at this point that a deep flexor tenotomy may need to be performed as this rapid progression is very concerning. Ideally a repeat venogram in another 4-7 days would have been best but finances limited to a 30 day check. Knowing what I know now about this case I would have cut tendons on day five and never looked back. Below is the Day one venogram on the left compared to the Day five Venograms on the right side. Focus your eyes on the circuflex artery, terminal papillae and the vasculature directly below the tip of coffin bone. Moderate compression and diplacement of these vessels five days into the syndrome. Remember that no measurable rotation, increase in h/l zones, loss of sole depth has occured.
After applying the modified ultimates on day one the horse began to make a clinical improvement noted by moving around in stall better and better appetite. He no longer rocked back to make turns. This is important to consider as clinical signs alone are not good indicators of how the case is going. The horse will lie to you when comes to laminitis.
 |
| Right Front venogram comparson Day one to Day five |
 |
| Left Front Venogram comparsion Day one to Day five. |
 |
| Day 5 |
 |
| Day five |
Below are venograms that are 30 days post laminitis of the left front. Note the circumflex is several milimeters above the tip of the coffin bone and no papillae are present. I again recommended deep flexor tenotomy as the modified ultimates are not providing enough mechanical relief, through unloading the force of the deep flexor. The tenotomy abolishes all forces applied to the bone to hoof attachments and solar corium directly below tip of coffin bone. Finances prohibited the Owner from going the surgical route and horse was actually improving with regard to pain and we decided to wait another thirty days.
 |
| 30 Days Post. The Circumflex artery is displaced several mm above the tip of the coffin bone and the solar vasculature is tightly compressed below the tip of the coffin bone. |
Below are 60 day post radiographs. Note the increased C/E distance, diverging H/L zones (rotation),and loss of sole depth, especially on the Left. No growth is noted on examination of the dorsal hoof wall and about 1/4 in at the heels is noted. Just to recap, we have no measurable displacement of the bone until 60 days into the syndrome but significant vascular changes on day five that continues to fail despite mechanical therapy. If you are waiting to diagnose laminitis based on rotation you are 60 days late in this case.
 |
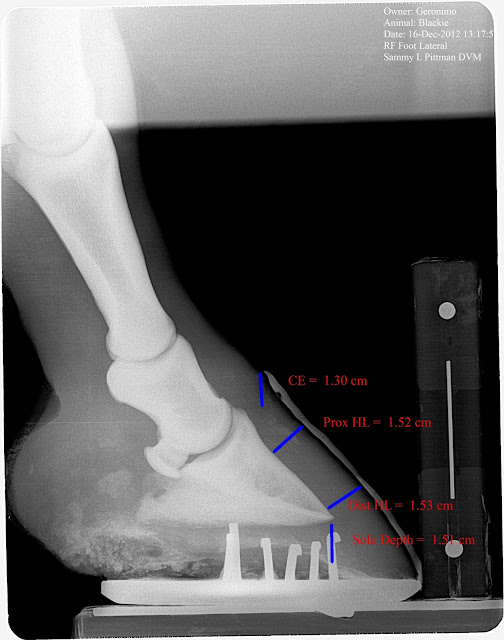
| 60 day post insult radiograph. Note changes in ce, hl zones and sole depth. |
 |
| 60 Days post initial insult. Note diverging hl zones (some may call rotation) increased in ce and comparable decrease in sole depth. |
Below are comparative venograms of the left front. On the left is day one and on the right is 90 days after intial insult. Note the greatly altered circumflex architecture and the tip of the coffin bone is visualized below the solar vessels. Moderate thickening of the dorsal sublamellar zone and significant accumalation of contrast as the dorsal coronary band that is likely secondary to a septic process that is brewing. Horse still has not grown any sole or dorsal hoof wall in 90 days. Note the scallop like loss of bone that occurs just above the tip caused by displacement of the terminal papillae and circumflex artery. I can only assume the combination of local hydraulic pressure and possibly the redirected papillae in this area are to blame for this unique change in the shape. At this stage in the game many irreversible changes have occurred that will likely prevent this horse from returning to a previous level of competition.
 |
| 90 days post comparison |
 |
| 90 days post comparison . The right foot has suffered less but prominent and significant change/damage has occurred in the area of the circumflex artery and terminal papillae. |
 |
| Left front Post tenotomy and derotation. |
 |
| Right Front post tenotomy and derotation. |
At the 90 day examination I advised the client that surgery was the only option for treatment and this late in the game I could only offer a guarded prognosis for any return to previous level of performance. The owner opted to donate the horse for a learning seminar. On March 22, 2012 a little over 90 days post initial insult a eager bunch of vet students and farriers performed venograms, applied derotation shoes and performed deep flexor tenotomies. In the days following the horse is moving much better. I will post followup radiographs in 30 days to evaluate the progress. I do feel recovery is still very likely. Ideally performing the tenotomy prior to irreversible damage and bone change would result in a better outcome.
1) In hindsight a deep flexor tenotomy should have been performed on day five or very shortly after.
2) Improvement with regards to pain and movement are not good indicators of success in laminitis.
3) Radiographic measurements alone, early in the syndrome, may change very little if any and a venogram may be the only information alluding to the nature of the insult.
4) Aggressive early mechanical therapy did relieve a lot of pain but did not provide enough unloading of the Deep digital flexor to aid in unloading of the vascular supply and further unloading via deep flexor tenotomy would have likely given a better outcome if performed earlier.
Stay tuned!

No comments:
Post a Comment