* Consultations * Laminitis/Founder * Thin soles * Navicular * Crushed/Low Heels * Foal development * Club feet * High Low Syndrome * Angular limb deformities
Welcome, About us
Hello and welcome. My name is Sammy L. Pittman, DVM and I am a veterinarian, farrier, and horsemen with a great interest in the field of equine podiatry. My wife and I own and operate Innovative Equine Podiatry and Veterinary Services in Collinsville TX. My passion lies within the health and well being of the hoof to better serve your equine companion. With so much lameness attributed to the lower limb many horses require an out of the box approach to achieve the success desired.
Give us a call and we will be glad to help you in any way we can. Thanks so much.
I will be discussing different Cases and thoughts from our world with the horse. Feel free to contact us via text or call at 903-718-0056 or send an email to iepvs11@gmail.com. Thank you for reading and enjoy
Pages
Monday, June 24, 2013
Friday, May 31, 2013
Hoof wall resection and update on Blackie the laminitis case.
Below are radiographs from immediately post deep flexor tenotomy and 60 days post tenotomy. Noteworthy change on both are additional sole depth under tip of coffin bone. However continued remodelling of the tip of the coffin bone and a slight increase in palmar angle on the left hoof are suggestive that the dorsal portion still fails to grow at a rate similar to the palmar portion. This hoof suffered more damage as it was the "club". Deep flexor tenotomy was not performed at the recommended time. Significant pathology was identified within 5 days of onset of acute laminitis but owner refused tenotomy at that time.
A resection is required in laminitis cases that have coronary band swelling that is prolapsing over the hoof wall. The hoof will act as a tourniquet as the inner laminae experience swelling. The lack of expansion of the hoof creates massive vascular compression and starves the laminae and coffin bone of needed nutrient flow. Often times this is all secondary to inflammation arising from compromised soft tissue and bone along the toe and medial quarter as this area tends to receive the most significant load induced vascular compromise when laminae fail to suspend the coffin bone.
I like to use a cast cutter or multi-purpose oscillating saw to cut through the hoof. Usually an 1 1/2 in below the hairline is a minimum and often times I find myself removing more at a later date. The width of resection will depend on amount of coronary band involved and should extend at least 1/2 in wider than the affected coronary band.
Next I use a sharp hook on the end of hoof knife to round and smooth the proximal (upper) edge of the intact hoof wall. It is important to perform this prior to removing hoof wall because it will get somewhat bloody after removal and occlude good visualisation.
Next the hoof wall can easily be removed by grasping one end with half rounds or regular nippers. Ease of removal is directly related timing of resection. Resections based on early evidence from venograms are usually more attached versus the case that has already separated and has drainage.
One removed, a gentle massage of the coronary papillae and lamina to encourage hemorrhage and lay the papillae in a more normal position pointing downward. Note the lack of hemorrhage in the most compromised region.
Next 1/2 inch felt heavily coated in silvadene cream is cut to fit the void left behind. This is tightly wrapped with elastikon as adequate pressure is important to prevent excessive swelling and granulation. Many times with cases that are far away and I am uncomfortable with the owners ability to maintain a bandage, I will place a cast over the elastikon up to the fetlock to maintain adequate compression. Preferably, daily changing for the first three days to ensure adequate hoof wall has been removed is recommended. After that a cast can be applied and changed every 7-10 days or bandage changes every 3-4 days. Each time a new piece of felt is applied with a fresh layer of silvadene. I will also use dmso gel applied to the coronary band to aid with inflammation.
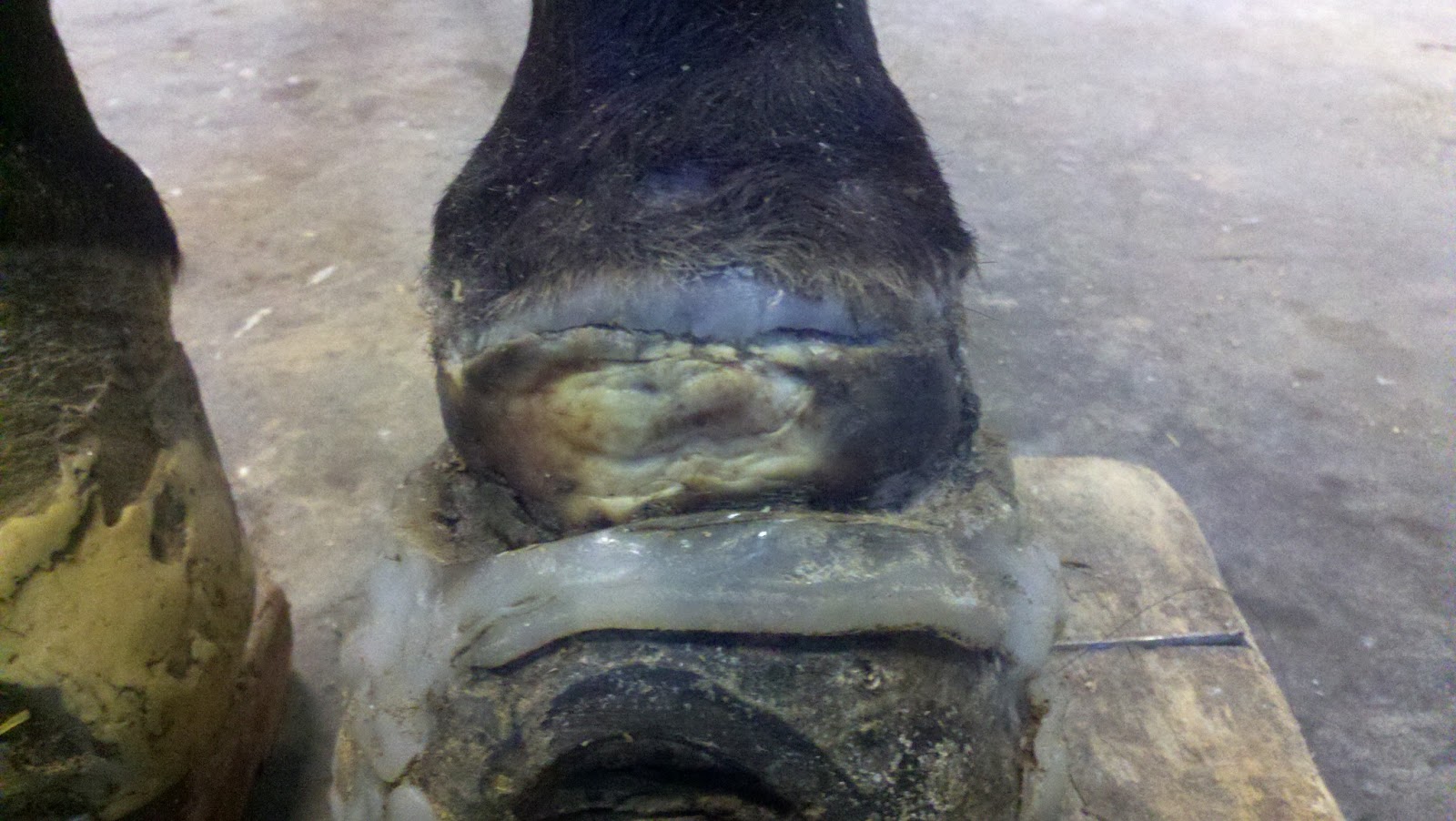
Images below are representative of what the hoof will look like at bandage or cast changes. This will depend greatly on the amount damage or compromise present. This case has significant damage with a lot of granulation already present. Ideally a resection should have been performed much earlier to prevent this level of damage to the coronary papillae. The first thing you will see is secretion of the secondary matrix horn which signifies the cornification process. Once this has covered the entire resection site, compression bandaging can be stopped and patient can go without any bandage at all. I like to see the cornification at the level of the previous hoof wall prior to stoppage of bandaging or casting.
Below are images of 5 days post resection. Notice the medial (inside) and lateral (outside) portions have already began to fill in with secondary matrix horn. The central portion suffered so much damage that the lamina are dead and unable to secrete matrix. This will fill and contract very similar to a wound anywhere else on the body via epithelialisation. A moist environment maintained with bandaging and/or cast will expedite the process.
Below are images from approximately 15 days later. A cast was placed over felt pad and elastikon for this period. Note the matrix is at the level of the hoof wall at the medial and lateral aspects and the granulation is reduced to 1/3.
These images are approximately 30 days post resection. Continued epithelialisation and secondary horn formation aka cornification.
Images below are about 6 weeks post resection and complete epithelialisation and cornification has occurred. At this point it is no longer necessary to apply cast or compressive bandages unless coronary band begins to get inflamed again.
Labels:
deep flexor tenotomy,
equine podiatry,
founder,
Hoof wall resection,
laminitis,
Sammy L Pittman DVM,
venograms
Collinsville texas
4181 North Osage Drive, Tulsa, OK 74127, USA
Thursday, May 30, 2013
New navicular case study
This is a 9 year quarter horse gelding that has had lameness issues since he was 3-4 years old. He has never been used outside of light training. I feel this type of navicular bone disease must have a genetic component as lesions where noted at an early age. This horse responded early on to low level mechanics that included a four point style shoe with digital breakover at the tip of p3. It progressed to needing significant mechanical enhancement but did respond to the enhanced mechanics applied via a rockered 4 point rail shoe. The horse was 4/5 bilateral lame on front before shoeing and 1/5 immediately post shoeing. A significant improvement was noted after the below shoeing method. The horse was euthanized due severity of disease and dissection was performed to further evaluate the navicular bone and compare to the radiographs. You will see below the lucent lesions noted in the high beam dorsopalmar radiographs and the 65 dg dorsopalmar radiographs. These lesions are present on the flexor surface of the navicular bone in which interacts with the flexor tendon. Note the tissue protruding from the lesions. This is tendonious tissue that has grown into the tendon and anchors the tendon to the navicular bone. I can imagine that at lower palmar angle the attachment tugging at the navicular bone lesions is terribly painful. This also explains why an increase in palmar angle and reduced digital breakover that reduced leverage and tension on the DDFT is so very helpful in this situation.
Many medical therapies are used in treatment of navicular disease however without appropriate mechancial treatment many medical therapies only offer temporary relief. Bursa injections, coffin joint injections, isoxoprine and tildren are common treatments. But you can see that without mechanical therapy that offers appropriate physical relief it can be difficult to manage. Cases like this can be difficult to manage at a performance level long term with mechanics and medical therapies and all but impossible without mechanical therapy.
The above drawing shows the ddft (green) coursing over the navicular to attach to the palmar surface of the coffin bone. The adhesions (red) are drawn in between the flexor surface and the tendon.
Below are pre- and post-shoeing radiographs. Note the drastic changes in palmar angle, tendon surface angle and distance of navicular bone to the condyle of proximal second phalanx (short pastern). In the rocker shoe the system is now a self adjusting mechanism with greatly decreased load on lesions and a greatly reduced leverage on the ddft. Again, this horse's lameness improved at least 80 percent with application of this shoe.
Many medical therapies are used in treatment of navicular disease however without appropriate mechancial treatment many medical therapies only offer temporary relief. Bursa injections, coffin joint injections, isoxoprine and tildren are common treatments. But you can see that without mechanical therapy that offers appropriate physical relief it can be difficult to manage. Cases like this can be difficult to manage at a performance level long term with mechanics and medical therapies and all but impossible without mechanical therapy.
Note the lucent regions on the radiographs and the corresponding lesion below. The tendon has grown into the navicular bone secondary to years worth of the tendon rubbing against the roughened flexor surface of the navicular bone. This causes abrasions on the tendon that leads to the adhesions connecting it to the navicular bone.
 |
| Viewing from front of hoof with navicular bone flipped up to expose the flexor (back) surface of the navicular bone in which the tendon glides over then attaches to coffin bone. |
 |
| Note the two adhesions on flexor surface. These where cut away from tendon |
 |
| This drawing shows the DDFT in green and adhesions in red |
Below are pre- and post-shoeing radiographs. Note the drastic changes in palmar angle, tendon surface angle and distance of navicular bone to the condyle of proximal second phalanx (short pastern). In the rocker shoe the system is now a self adjusting mechanism with greatly decreased load on lesions and a greatly reduced leverage on the ddft. Again, this horse's lameness improved at least 80 percent with application of this shoe.
Monday, March 25, 2013
Acute laminitis case showing the value of the venogram
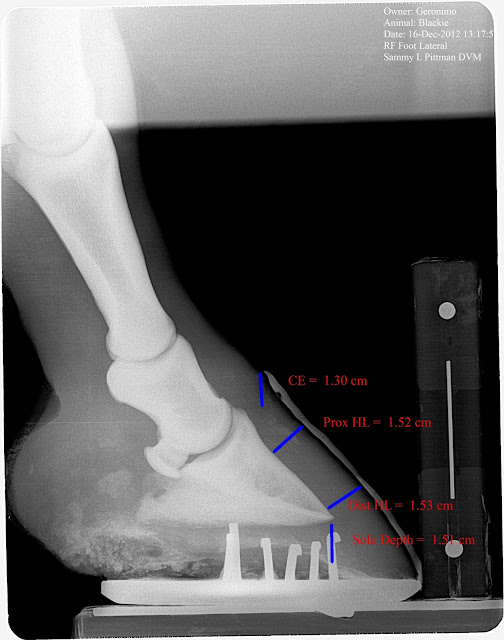
This is an acute laminitis case that was initially painful and exhibiting the typical founder stance on December 16 2012. No known cause but a mild colic episode had occurred 3 days prior. I was able to perform venograms on what I would consider Day one of laminitis. These plain film radiographs and venograms create a baseline in which to compare follow up venograms. This allows assesment of the mechanical therapy applied and severity of compromise in the days to follow. Venograms 5 days later show moderate compromise already. Consider the amount of compromise present while treated with mechanics. Unloading the Deep flexor tendon, its forces applied to the dorsal lamellar zone and sole directly below tip of coffin bone via raising the palmar angle.
There is no measurable displacement of the bone but significant change has occured within the vascular network as early as five days. Some financial constraints existed and it was decided to wait 30 days and repeat venograms to evaluate if the mechanics applied would be enough. I warned the client at this point that a deep flexor tenotomy may need to be performed as this rapid progression is very concerning. Ideally a repeat venogram in another 4-7 days would have been best but finances limited to a 30 day check. Knowing what I know now about this case I would have cut tendons on day five and never looked back. Below is the Day one venogram on the left compared to the Day five Venograms on the right side. Focus your eyes on the circuflex artery, terminal papillae and the vasculature directly below the tip of coffin bone. Moderate compression and diplacement of these vessels five days into the syndrome. Remember that no measurable rotation, increase in h/l zones, loss of sole depth has occured.
After applying the modified ultimates on day one the horse began to make a clinical improvement noted by moving around in stall better and better appetite. He no longer rocked back to make turns. This is important to consider as clinical signs alone are not good indicators of how the case is going. The horse will lie to you when comes to laminitis.
 |
| Right Front venogram comparson Day one to Day five |
 |
| Left Front Venogram comparsion Day one to Day five. |
 |
| Day 5 |
 |
| Day five |
Below are venograms that are 30 days post laminitis of the left front. Note the circumflex is several milimeters above the tip of the coffin bone and no papillae are present. I again recommended deep flexor tenotomy as the modified ultimates are not providing enough mechanical relief, through unloading the force of the deep flexor. The tenotomy abolishes all forces applied to the bone to hoof attachments and solar corium directly below tip of coffin bone. Finances prohibited the Owner from going the surgical route and horse was actually improving with regard to pain and we decided to wait another thirty days.
 |
| 30 Days Post. The Circumflex artery is displaced several mm above the tip of the coffin bone and the solar vasculature is tightly compressed below the tip of the coffin bone. |
Below are 60 day post radiographs. Note the increased C/E distance, diverging H/L zones (rotation),and loss of sole depth, especially on the Left. No growth is noted on examination of the dorsal hoof wall and about 1/4 in at the heels is noted. Just to recap, we have no measurable displacement of the bone until 60 days into the syndrome but significant vascular changes on day five that continues to fail despite mechanical therapy. If you are waiting to diagnose laminitis based on rotation you are 60 days late in this case.
 |
| 60 day post insult radiograph. Note changes in ce, hl zones and sole depth. |
 |
| 60 Days post initial insult. Note diverging hl zones (some may call rotation) increased in ce and comparable decrease in sole depth. |
Below are comparative venograms of the left front. On the left is day one and on the right is 90 days after intial insult. Note the greatly altered circumflex architecture and the tip of the coffin bone is visualized below the solar vessels. Moderate thickening of the dorsal sublamellar zone and significant accumalation of contrast as the dorsal coronary band that is likely secondary to a septic process that is brewing. Horse still has not grown any sole or dorsal hoof wall in 90 days. Note the scallop like loss of bone that occurs just above the tip caused by displacement of the terminal papillae and circumflex artery. I can only assume the combination of local hydraulic pressure and possibly the redirected papillae in this area are to blame for this unique change in the shape. At this stage in the game many irreversible changes have occurred that will likely prevent this horse from returning to a previous level of competition.
 |
| 90 days post comparison |
 |
| 90 days post comparison . The right foot has suffered less but prominent and significant change/damage has occurred in the area of the circumflex artery and terminal papillae. |
 |
| Left front Post tenotomy and derotation. |
 |
| Right Front post tenotomy and derotation. |
At the 90 day examination I advised the client that surgery was the only option for treatment and this late in the game I could only offer a guarded prognosis for any return to previous level of performance. The owner opted to donate the horse for a learning seminar. On March 22, 2012 a little over 90 days post initial insult a eager bunch of vet students and farriers performed venograms, applied derotation shoes and performed deep flexor tenotomies. In the days following the horse is moving much better. I will post followup radiographs in 30 days to evaluate the progress. I do feel recovery is still very likely. Ideally performing the tenotomy prior to irreversible damage and bone change would result in a better outcome.
1) In hindsight a deep flexor tenotomy should have been performed on day five or very shortly after.
2) Improvement with regards to pain and movement are not good indicators of success in laminitis.
3) Radiographic measurements alone, early in the syndrome, may change very little if any and a venogram may be the only information alluding to the nature of the insult.
4) Aggressive early mechanical therapy did relieve a lot of pain but did not provide enough unloading of the Deep digital flexor to aid in unloading of the vascular supply and further unloading via deep flexor tenotomy would have likely given a better outcome if performed earlier.
Stay tuned!
Subscribe to:
Comments (Atom)